Heart Failure and the Glenn - June 4, 1998
(And Ben, from 3 - 6 1/2 months)
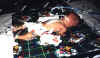
On Thursday, June 4, 1998, I got home from work around 6pm. Benjamin was acting a little strange and would not nurse. We went to our daughter, Nicole's, play at her school, and while we were there, I started to feel something was terribly wrong with Ben. Normally so smily, he just laid in my arms and stared off into space. He did not wiggle or anything. I could not wait for Nicole's play to finish.At 9pm, we phoned the Children's Heart Clinic. Dr. Cabalka told us to come to the ER. When we got there, Ben's oxygen saturation levels (sats) were only 62%. Just two days earlier, they had been 82%. We were told Ben was in severe congestive heart failure and would need to be admitted. We were in shock. This had all come on so fast.
Ben was admitted to PICU at Childrens Hospital in Minneapolis again. He was immediately put on the ventilator to ease the load on his heart. What appeared to have happened was when the balloon angioplasty was done two days earlier, the increased blood flow was too much for Ben's right ventricle, his only pumping chamber. Instead of pumping the blood out to the body and lungs as it came into the heart, the heart simply grew bigger and bigger. Upon being intubated, Ben's heart was beating 210 times a minute.
With the use of dopamine and nypride, the PICU staff was able to get Ben's heart rate and blood pressure down. It was so hard to be back in the hospital, especially with Ben in such critical condition.
When Dr. Singh, our cardiologist, came in on Friday (6/5) morning, he was shocked to see us there. He had just seen Ben on Tuesday, and everything looked good.
Dr. Singh and Dr. Helseth discussed Ben's situation. It looked as though the Glenn procedure would have to be done now. The Glenn would connect the superior vena cava directly to the pulmonary arteries, which flow directly to the lungs. This would mean that the lungs would get blood simply by gravity. The heart would not have to pump the blood to the lungs, and therefore, would not have to work so hard. The hopes were that once the heart did not have to work so hard, it could be strengthened and continue to pump blood to the body. The surgery was scheduled for the following morning.
Surgery went very well. Ben was only on bypass for 36 minutes. We were allowed to see Ben less than four hours after they had wheeled him away. It was interesting how this time, we did not really see all the tubes on Ben (although they were there). This time, we saw Ben. Last time, it was hard to see past the wires.
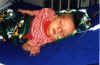
6/7/98 - One day after surgery |
Benjamin, just moments after being taken off the ventilator - 6/9/98 |
The doctors decided to start Ben on a methadone wean. This would help ease his withdrawal. It seemed to start working by Wednesday evening, because Ben finally fell asleep. At 2am on Thursday morning, we were moved out of PICU to the general pediatrics floor. The PICU was full, and they needed the room. Ben would have moved up in the morning anyway, so it was not a big deal.
On Thursday (6/11) Ben was taken off all of his monitors, and all of his lines were removed. He was doing marvelous. On Friday (6/12), our wonderful cardiologist came into our room and said, “So, what do you think about going home today?” We were shocked, but excited. At 3pm, we were discharged, just one week after Ben had been admitted in severe congestive heart failure.
6/11/98 - One day before going home |
We are SO very thankful to the wonderful doctors and staff at Childrens. They are the most skilled, compassionate, wonderful people in the medical profession we have met, and we are deeply grateful to be in their care. A special thanks to Dr. Singh, Dr. Helseth, Dr. Solfelt, Dr. Cabalka, Peggy, Shannon, Jeanie, Kandi, Ginger, Kathy W., Jane, Beth and everyone else who cared for Ben (and us)! We can never really express the depth of our appreciation for all you have done for us!!
6/25/98 - 3 1/2 months old
Finally, after 2 weeks of crying following surgery, we get a smile!! |
|
Ben loves his swing. |
7/29/98 - 4 1/2 months old
We are going on three weeks without having to be in the hospital, at the clinic or on the phone with Benjamin's pediatrician or cardiologist!! This is a real blessing after we struggled through the month of June.
With the heart cath, heart failure, the Glenn procedure, and 2-3 weeks of constant crying, there were only three days the entire month we weren't in contact with someone at the hospital or clinic. June was by far the toughest month for us since Ben was born. We were re-hospitalized after he went home for the Glenn due to his uncontrollable crying. We were given several possible reasons for the crying, although nothing definite. After a month on phenobarb, a drug often used to control seizures (which Ben did not have), Ben seems to be coming around. He is now off all medications except digoxin, which is the drug used to make his heart beat stronger, but slower. Ben's next appointment is 8/7/98, and if all goes well, we won't have to go back for THREE MONTHS!!!!!!
Ben is really developing well. He's eating good, gaining weight and smiling all the time. Just last week he began to reach for his toys, and yesterday I caught him holding onto his toes and staring at them like they were the neatest thing he'd ever seen! He also slept through the night for the first time last night, at least the first time that was not drug induced.
We marvel at the blessing God has given us, and treasure every day we have with him, not knowing or thinking about what the future holds. No one is guaranteed tomorrow, so we must live for today!
08/11/98 - 5 months old
Benjamin had a wonderful checkup last week! His sats were holding at 82%, his coarctation (narrowing) of the aorta has remained open and does not currently require surgery, and he weighed in at a hefty 12lbs. 10ozs! We do not need to return for another checkup for two full months!
09/20/98 - 6 1/2 months old
Well, we didn't make it our two months between visits. Last Wednesday (9/17/98), Ben started making grunting noises when he was crying. He has been very whiny the last month or so, but we thought it might be his teeth coming in. After his grunting spell, he fell asleep for a few minutes. When he awoke, we saw that very familiar blank stare. It was the same stare he gave us in June when he was in heart failure. No clapping, finger snapping, or yelling would cause him to react. We rushed him to the E.R. at Children's Hospital.
As the night went on, the doctor on call decided it might be more abdominal related, because Ben became very upset when the doctor pushed around his abdomen. The chest xray came back, and it did not appear that Ben's heart was any larger (a key sign of heart failure.) We were admitted for the night.
In the morning, Dr. Cabalka had an echo done, and it clearly showed that Ben's aorta was again narrowed. It was about 10mm above and below the narrowing, but just 2-3mm wide at the narrowing.
Our cardiologist is out of town, but will be back in time for surgery, which is scheduled for Wednesday, 9/23, at 10am. Although there still may be something wrong in his abdomen area, we need to fix the aorta first. If his sensitivity in this area continues, we will pursue it further.